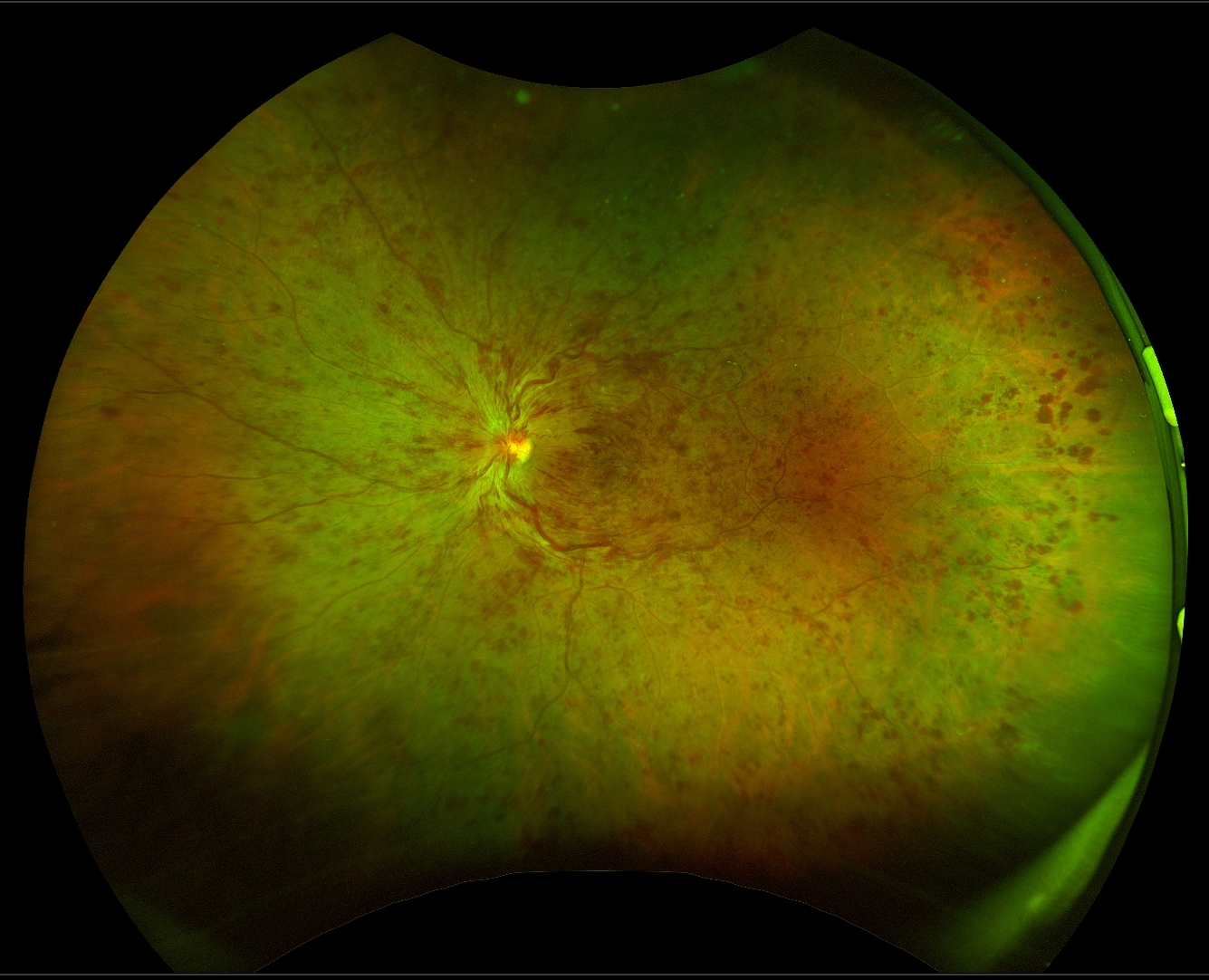
In addition, the superior-temporal detachment that ultimately occurred was not evident in the earlier photographs. One of us (JS) opined that the practitioner performed a standard-of-care examination and that, based on the photos, a detachment was not evident. This case is unusual because, unbeknownst to both of us, we were each asked to opine for opposite sides. If the practitioner did not see a detachment, should the patient have been referred to a retina specialist for supplementary testing procedures, such as scleral depression, three-mirror contact lens examination and/or B-scan ultrasonography? Should the practitioner have made a follow-up appointment after the initial examination? Our Opinion Do you see a retinal detachment in Figure 1? Was there a retinal detachment when the patient initially complained of a shadow? The practitioner did not see a detachment but took photos. The patient claimed that the failure to detect the detachment on the day he was experiencing the shadow delayed treatment, resulting in a macula-off retinal detachment and two surgeries, which resulted in irreversible reduction of vision in the right eye with distortions in his vision that he claimed made it difficult to perform his construction work. The patient initiated a malpractice lawsuit against the practitioner for failure to diagnose the retinal detachment when he initially complained of the shadow and for failure to refer him to a retina specialist for prompt treatment. A membrane peel was recommended, as was cataract extraction.įive months later, the best-corrected visual acuity remained 20/60 in the right eye. The patient was noted to have developed a 2+ nuclear and posterior subcapsular cataract (secondary to the vitrectomy performed during the retinal repair) and a new epiretinal membrane with macular edema. Two months later, the patient reported that images appeared “bent” in the center of vision in his right eye when performing daily tasks. One month later, the visual acuity had improved to 20/80, and the patient reported that the vision was still distorted. The detachment was repaired one day later. The patient was immediately referred to a retina specialist, who diagnosed a superior-temporal tear and a large bullous macula-off retinal detachment. Examination revealed a large retinal detachment ( Figure 2). Visual acuity in the right eye was hand motion. The patient returned one month later with a complaint that he woke up with reduced vision in the right eye only that morning and that he had had flashes and floaters, which had started two days before. The retinal specialist described a superior-temporal macula-off retinal detachment. The patient was diagnosed with a shadow “due to new vitreal strands and a new PVD.” The practitioner wrote “reviewed retinal detachment, the signs and symptoms today…” No return appointment was scheduled.įig. Several Optos photographs were taken using steering with emphasis on the temporal retina ( Figure 1). The dilated fundus examination was performed, and the practitioner noted “new and large vitreal strands OD.”īecause of the specificity of the patient’s new complaint about the shadow being more obvious when he looked to the right, the practitioner was more suspicious of a problem in the temporal retina of the right eye (nasal field). The patient was dilated with 1.0% tropicamide and 2.5% phenylephrine. Biomicroscopy was performed but the practitioner did not note the presence or absence of pigmented cells in the vitreous, the so-called “Schafer’s sign,” which can indicate the possible presence of a retinal tear. No anterior segment abnormalities were noted. The practitioner noted uncorrected visual acuities of 20/40 in each eye but not corrected acuities. Optos photo of the right eye, with two cortical spokes nasally and a wide one superior temporal. The practitioner wrote “patient started seeing a shadow in the left side of the right eye it is there when looking to the right, not as much looking straight or to the left.” The practitioner noted “no flashes, history of floaters.”įig.1. Six months after his last follow-up, he presented with a different complaint. At each visit the patient deferred dilation. For the next year, the patient was followed for three visits related to contact lenses and dry eye secondary to the LASIK.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
